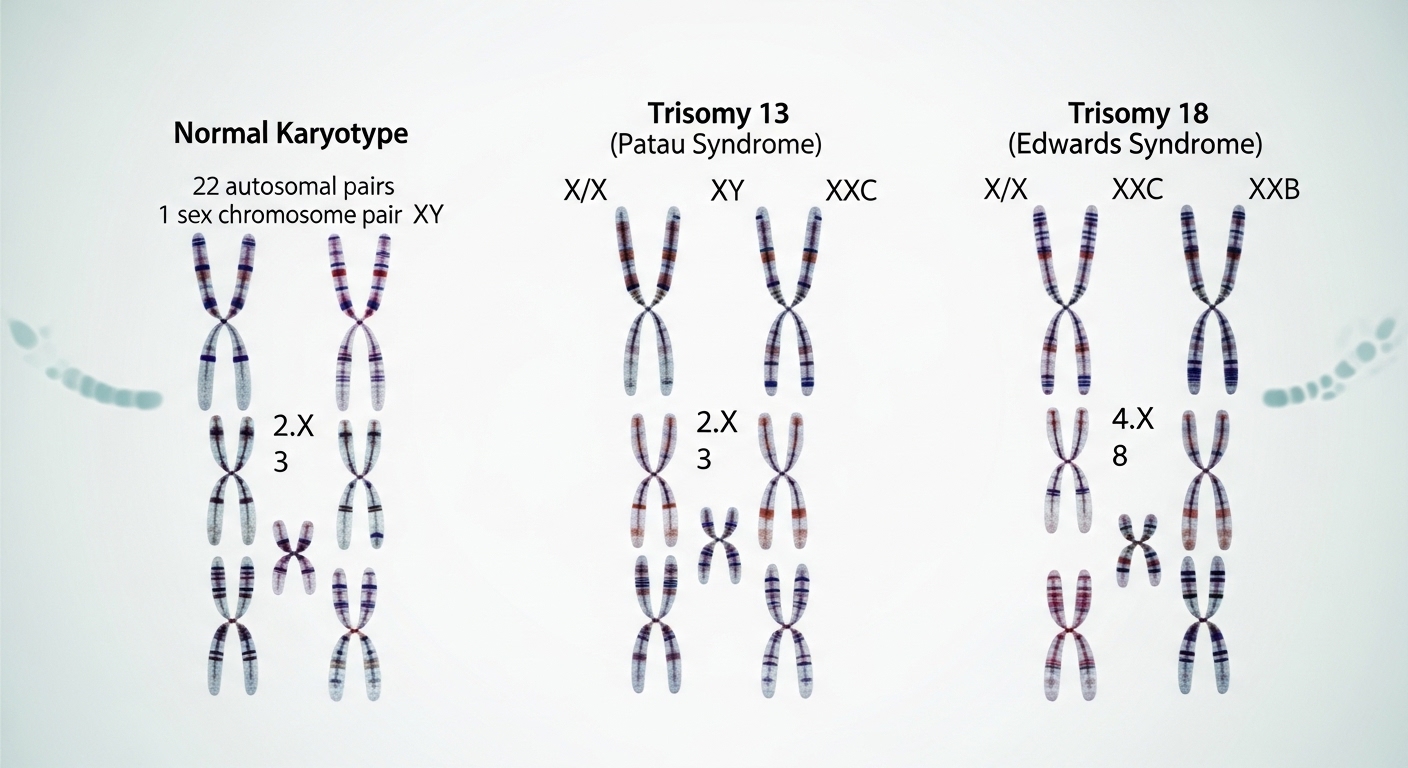
Patau syndrome (Trisomy 13) and Edwards syndrome (Trisomy 18) are serious chromosomal conditions that occur when a fetus has an extra copy of chromosome 13 or 18, leading to severe developmental abnormalities, pregnancy complications, and a high risk of stillbirth or early infant death.
Many expecting parents first hear these terms during prenatal screening and immediately feel uncertainty and fear. These diagnoses are rare but medically significant because they affect multiple organs, growth patterns, and survival outcomes. Understanding what they mean—and what options exist—helps families make informed decisions during pregnancy.
This guide explains how these conditions happen, how they are detected, what they mean for pregnancy outcomes, and what support pathways exist after diagnosis.
Why Are Patau Syndrome and Edwards Syndrome Important to Understand During Pregnancy?
These syndromes are important to understand because they significantly affect fetal survival, pregnancy management decisions, and counseling options for parents.
Prenatal screening now detects chromosomal differences earlier than ever. Conditions like Trisomy 13 and Trisomy 18 are often identified in the first or second trimester through ultrasound markers and blood tests. Early detection allows families and clinicians to prepare medically, emotionally, and ethically.
Globally:
- Trisomy 18 occurs in approximately 1 in 5,000 live births
- Trisomy 13 occurs in about 1 in 10,000–16,000 live births
- Most affected pregnancies end in miscarriage or stillbirth
- Less than 10% of infants survive beyond the first year
These statistics highlight why early recognition matters.
What Is Patau Syndrome (Trisomy 13)?
Patau syndrome is a genetic condition caused by an extra copy of chromosome 13 that disrupts normal fetal development and affects the brain, heart, and facial structure.
Chromosome 13 contains genes responsible for early organ formation. When an extra copy exists, cells receive incorrect developmental instructions. This leads to multiple structural abnormalities.
Common features include:
- Cleft lip or palate
- Extra fingers or toes (polydactyly)
- Severe brain abnormalities
- Heart defects
- Small eyes or missing eye structures
- Kidney malformations
Many pregnancies affected by Trisomy 13 end before birth. Among live births, survival beyond several months is uncommon.
What Is Edwards Syndrome (Trisomy 18)?
Edwards syndrome is a chromosomal condition caused by an extra chromosome 18 that leads to restricted growth, organ defects, and severe developmental delays.
This syndrome affects nearly every organ system. Unlike Trisomy 13, physical growth restriction is often one of the earliest detectable signs.
Typical characteristics include:
- Low birth weight
- Small jaw (micrognathia)
- Overlapping fingers
- Heart abnormalities
- Kidney problems
- Rocker-bottom feet
Pregnancies with Trisomy 18 frequently involve complications such as reduced fetal movement and placental insufficiency.
What Causes Trisomy 13 and Trisomy 18 in Pregnancy?
Both conditions are caused by nondisjunction, a genetic error where chromosomes fail to separate properly during egg or sperm formation.
Normally, embryos inherit two copies of each chromosome. In trisomy conditions, three copies are present instead. This extra genetic material disrupts normal development.
There are three types:
Full Trisomy
Every cell carries an extra chromosome. This is the most severe and most common form.
Mosaic Trisomy
Only some cells carry the extra chromosome. Symptoms may be milder depending on distribution.
Partial Trisomy
Only part of the chromosome is duplicated. Effects vary widely.
Maternal age increases risk, but these conditions can occur in pregnancies at any age.
How Are Patau Syndrome and Edwards Syndrome Detected During Pregnancy?
These conditions are usually detected through prenatal screening tests followed by confirmatory diagnostic procedures.
Screening methods estimate risk rather than providing certainty.
First Trimester Screening
- Nuchal translucency ultrasound
- Maternal blood markers
- Combined risk assessment models
Non-Invasive Prenatal Testing (NIPT)
NIPT analyzes fetal DNA fragments in maternal blood and can detect Trisomy 13 and 18 with high sensitivity.
Second Trimester Ultrasound
Structural abnormalities often appear during anomaly scans between 18–22 weeks.
Diagnostic Confirmation Tests
- Chorionic villus sampling (CVS)
- Amniocentesis
These tests confirm chromosomal status with near certainty.
What Ultrasound Signs Suggest Trisomy 13 or Trisomy 18?
Ultrasound may reveal structural abnormalities such as growth restriction, brain defects, heart anomalies, or limb positioning differences that suggest chromosomal syndromes.
Common indicators include:
- Increased nuchal translucency
- Holoprosencephaly (brain development issue)
- Clenched hands
- Single umbilical artery
- Omphalocele
- Congenital heart defects
Detection often prompts further genetic testing.
How Do Patau Syndrome and Edwards Syndrome Affect Pregnancy Outcomes?
Both conditions significantly increase the likelihood of miscarriage, stillbirth, premature delivery, and neonatal complications.
Pregnancy complications may include:
- Polyhydramnios (excess amniotic fluid)
- Poor fetal growth
- Placental dysfunction
- Reduced fetal movement
- Preterm labor
Because survival rates are limited, pregnancy care plans often involve specialized counseling.
What Is the Difference Between Patau Syndrome and Edwards Syndrome?
The main difference is the chromosome affected—Trisomy 13 impacts chromosome 13, while Trisomy 18 affects chromosome 18—and each condition produces distinct physical abnormalities and survival outcomes.
| Feature | Patau Syndrome (Trisomy 13) | Edwards Syndrome (Trisomy 18) |
|---|---|---|
| Affected Chromosome | Chromosome 13 | Chromosome 18 |
| Brain Abnormalities | Common and severe | Less frequent but present |
| Growth Restriction | Moderate | Severe |
| Hand Position | Extra fingers common | Clenched overlapping fingers |
| Survival Rate | Very low | Very low |
| Heart Defects | Common | Very common |
Can Babies With Trisomy 13 or Trisomy 18 Survive?
Some babies survive birth, but long-term survival beyond the first year is rare due to severe organ abnormalities.
Survival estimates:
- Over 90% of affected pregnancies end before or shortly after birth
- 5–10% survive beyond one year
- Mosaic cases may have longer survival
Medical support decisions vary depending on severity and family preferences.
What Are the Risk Factors for Trisomy 13 and Trisomy 18?
Advanced maternal age is the strongest known risk factor, although most cases occur randomly.
Additional risk contributors include:
- Previous trisomy pregnancy
- Chromosomal translocation in parents
- Maternal age above 35
- Rare genetic predispositions
Genetic counseling helps clarify recurrence risk.
What Should Parents Do After a Positive Screening Result?
Parents should confirm results with diagnostic testing and consult maternal-fetal medicine specialists for guidance on prognosis and options.
Recommended next steps:
- Confirm diagnosis with CVS or amniocentesis
- Consult a genetic counselor
- Discuss pregnancy continuation choices
- Plan delivery with a specialist team
- Explore neonatal care expectations
Accurate diagnosis supports informed decision-making.
Is There Treatment for Patau Syndrome or Edwards Syndrome Before Birth?
There is no cure before birth, but prenatal monitoring helps manage complications and prepare for delivery planning.
Care strategies may include:
- Frequent ultrasounds
- Growth monitoring
- Heart defect evaluation
- Delivery planning at tertiary hospitals
Supportive care improves coordination between specialists and families.
How Do Doctors Support Families After Diagnosis?
Healthcare teams provide counseling, medical planning guidance, and emotional support tailored to each family’s preferences and values.
Support typically includes:
- Genetic counseling sessions
- Perinatal palliative care consultation
- High-risk pregnancy monitoring
- Neonatal planning discussions
These services help families prepare for multiple possible outcomes.
Conclusion: What Should Expecting Parents Remember About Trisomy 13 and Trisomy 18?
Patau syndrome and Edwards syndrome are serious chromosomal conditions that affect fetal development, pregnancy outcomes, and neonatal survival, but early screening and informed counseling help parents navigate decisions with clarity.
Modern prenatal testing allows earlier detection than ever before. That means families can access specialist guidance, confirm diagnoses accurately, and plan next steps based on medical evidence rather than uncertainty.
If screening results raise concern, speak with a maternal-fetal medicine specialist or genetic counselor promptly. Understanding the condition is the first step toward making confident, informed choices for your pregnancy journey.
MedlinePlus (U.S. National Library of Medicine – .gov): Trisomy 13 (Patau Syndrome) and Trisomy 18 (Edwards Syndrome) — These provide comprehensive, trusted overviews of both conditions.
Frequently Asked Questions About Patau Syndrome and Edwards Syndrome in Pregnancy
Can Trisomy 13 or Trisomy 18 be prevented?
No, these conditions cannot be prevented because they result from random chromosomal separation errors during early embryo formation.
Are screening tests always accurate?
No, screening tests estimate probability rather than confirming diagnosis, which is why amniocentesis or CVS is required for certainty.
Does maternal age guarantee higher risk?
No, risk increases with maternal age but many affected pregnancies occur in younger women.
Can babies with mosaic trisomy live longer?
Yes, mosaic cases sometimes have milder symptoms and longer survival depending on how many cells are affected.
Is NIPT reliable for detecting Trisomy 13 and 18?
Yes, NIPT has high sensitivity for these conditions, though diagnostic testing is still required for confirmation.
Will future pregnancies have the same condition?
Most future pregnancies are unaffected, but recurrence risk depends on whether a parental chromosomal rearrangement exists.
Should genetic counseling be done after diagnosis?
Yes, genetic counseling helps families understand prognosis, recurrence risk, and available pregnancy management options.
Read More Also: Peptide Therapy: A Modern Approach to Wellness
Discover More: How to Improve Skin Clarity Through Daily Cleansing Habits